NO-SCALPEL VASECTOMY
Experience Gentle And Effective No-Scalpel Vasectomy In Perth

What Sets No-Scalpel Vasectomy Apart as a Safe Procedure
Traditional vasectomy methods typically involve small incisions and stitches, which may require a longer healing period. Some men may have concerns about post-procedure discomfort, infection, or recovery time.
A no-scalpel vasectomy uses a small puncture instead of an incision, aiming to reduce discomfort, infection risk, and downtime. While individual experiences vary, this method is designed to be a minimally invasive alternative to traditional vasectomy.

Why Choose Perth Vasectomy Centre?
Experience
Dr. Essa Rasool has years of extensive experience performing vasectomies, offering confidence and professionalism throughout the entire process.
Reputation
Since 2017, patients have trusted us to provide reliable vasectomy services in a professional, welcoming, and patient-centred environment.
Comfort
The no-scalpel technique reduces discomfort, speeds up recovery time, and minimises risks compared to traditional vasectomy methods.
Convenience
We are centrally located in Ascot and Baldivis, with flexible appointment times, same-day bookings, and onsite parking for easy access.
Affordability
We offer transparent pricing with Medicare rebates and no hidden fees, making our vasectomy services accessible and budget-friendly.
Aftercare
Comprehensive follow-up care is provided to address any concerns so that our patients feel supported and comfortable after their procedure.
A Gentle Process: The No-Scalpel Vasectomy Procedure Explained



Local Anaesthetic Administered for Comfort During the Procedure
Local anaesthetic is gently applied to numb the scrotal area, helping to manage discomfort during the procedure. This numbing effect allows patients to remain comfortable and awake throughout the treatment. The anaesthetic also aids in reducing sensitivity during recovery, which may contribute to a more comfortable healing experience.
Tiny Incision-free Entry Provides Access to Vas Deferens Safely
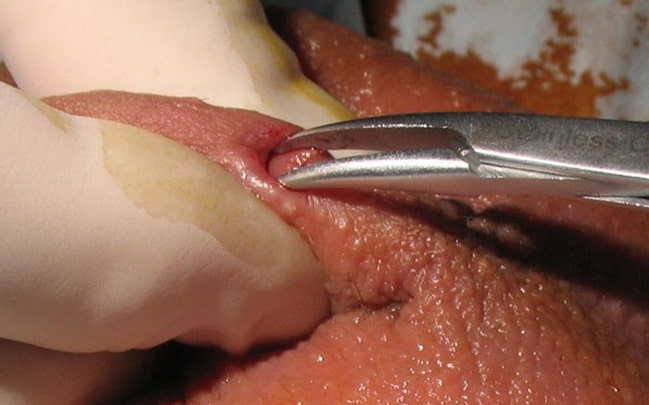
A sharp tool creates a small puncture in the scrotum, avoiding the need for incisions. This technique aims to reduce skin damage, lower infection risks, and provide safe, precise access to the vas deferens. The small puncture size may promote faster healing with potentially less swelling and minimal post-procedure discomfort compared to traditional vasectomy methods.
Sealing Vas Deferens with Precision to Prevent Sperm Travel
Perth Vasectomy Centre utilises fascial interposition to seal the vas deferens. This technique is designed to block sperm, reducing the likelihood of the tubes reconnecting and providing reliable long-term contraception. Fascial interposition adds an extra layer of security, helping to lower the chance of the vas deferens rejoining over time.
DOCTOR'S PROFILE
Meet Dr. Essa Rasool

Dr. Essa Rasool
GP Obstetrician
Dr. Essa Rasool is a highly experienced medical professional with a career spanning decades. He spent 26 years at Rockingham General Hospital, delivering babies and providing exceptional care. Obtained a Medical Degree at Royal College of Surgeons in Dublin Ireland. He also earned a diploma from the Royal College of Obstetricians and Gynaecologists.
Now practising at the Ridge Medical Centres both in Ascot and Baldivis, Dr. Rasool provides care in areas like men’s health and vasectomy. A Fellow of the Royal Australian College of General Practitioners, he has been performing vasectomies since 1990 under local anaesthetic.
Dr. Essa Rasool
GP Obstetrician
Patient Resources Designed to Guide You Through Your Vasectomy Journey

Answers to Frequently Asked Questions About Vasectomy for Confident and Informed Decision-Making
Essential Preparation Tips for a Successful Vasectomy Experience

Vasectomy Aftercare Made Simple With Expert Guidance and Support

Frequently Asked Questions
Got a question we missed? Contact Us
What is a no-scalpel vasectomy?
How does a no-scalpel vasectomy work?
The no-scalpel vasectomy is a simple, minimally invasive procedure performed under local anaesthesia. Here’s how it works:
The no-scalpel vasectomy is a simple, minimally invasive procedure performed under local anaesthesia. Here’s how it works:
- Preparation:
Patients discuss the procedure, risks, and alternative methods like tubal ligation. Possible complications, including post-vasectomy pain syndrome, are also reviewed. The scrotum is cleaned, and local anaesthetic is applied. - Puncture and access:
The vas deferens is located and stabilised. A sharp tool creates a small puncture, helping to reduce the risk of bleeding and infection. - Sealing the vas:
A section of the vas deferens may be removed to help reduce the likelihood of reconnection. The ends of the vas are then sealed using one of several techniques, including tying, cauterisation, fascial interposition, or the open-ended method.
At Perth Vasectomy Centre, fascial interposition is commonly used as an added layer of security to lower the likelihood of the tubes reconnecting. - Closure:
The vas is returned, and the puncture naturally heals without stitches.
Post-procedure care:
A small dressing is applied, and patients are monitored for any immediate concerns. A semen analysis after approximately 20 ejaculations or three months is required to confirm success.
Other forms of contraception must be used until sperm clearance is confirmed.
What is the difference between traditional and no-scalpel vasectomy (NSV)?
Both traditional vasectomy and the NSV method are highly effective forms of contraception, but they differ in key areas:
- Accessing the tubes carrying sperm:
- Traditional vasectomy: Doctors make two small incisions in the scrotum to access the vas deferens.
- NSV method: A sharp tool creates a small puncture in the scrotum, which may result in reduced skin wounds and tissue disruption.
- Procedure:
- Traditional vasectomy: The vas deferens is cut, and the ends are tied or sealed, with stitches required to close the incisions.
- NSV method: A small section of the vas deferens may be removed, and the ends are sealed using techniques like fascial interposition without requiring stitches.
- Healing:
- Traditional vasectomy: The healing process may take longer because stitches are needed, which can increase the risk of infection.
- NSV method: Recovery can be shorter because the puncture heals naturally without stitches, though individual healing times vary.
- Complication rates:
- Traditional vasectomy:
This method may carry a higher risk of bleeding, infection, and post-surgery discomfort. - NSV method:
Studies suggest the NSV method may reduce the risk of swelling, bleeding, and infection compared to traditional vasectomy, though all surgical procedures carry some risks.
- Traditional vasectomy:
- Failure rate:
- Both methods have a low failure rate, with no significant difference reported in studies.
- 6. Patient benefits:
- NSV method:
The NSV method is often chosen because it is less invasive, may allow for quicker healing, and results in fewer complications.
- NSV method:
Both methods are reliable options for contraception and do not impact sex drive. Patients considering future family planning options should discuss vasectomy reversal during consultation.
What is the success rate of a no-scalpel vasectomy?
The NSV is considered a highly effective form of long-term contraception, with studies reporting a success rate above 99% when performed the right way. Several factors contribute to its effectiveness:
- Blocking the vas deferens:
The tubes carrying sperm are cut, sealed, or tied to prevent sperm from mixing with semen, resulting in infertility once clearance is confirmed. - Semen testing:
A follow-up semen test is required to confirm the absence of sperm. Until then, alternative contraception must be used. - Doctor’s skill:
The success of the procedure depends on the doctor accurately identifying and sealing the vas deferens. - Aftercare compliance:
Following post-procedure instructions—including attending follow-up tests and avoiding strenuous activity—helps support the effectiveness of the procedure.
When done properly, an NSV is a reliable option for those who no longer wish to have children.
How big is the incision for a no-scalpel vasectomy?
What are the advantages of no-scalpel vasectomy?
The NSV technique has several potential advantages over traditional methods:
- Minimally invasive:
A small puncture replaces large incisions, which may help reduce skin trauma and eliminate the need for stitches, potentially supporting faster healing. - Lower risk of complications:
The small puncture may lower the chance of bleeding, swelling, or infection and allow access to the upper part of the vas deferens without the need for larger incisions. - Effective contraception:
The vas deferens is cut, tied, sealed, or cauterised to prevent sperm from mixing with semen. A follow-up semen analysis is required to confirm success. - Quick recovery:
The procedure is typically completed quickly, and many men resume normal activities within a few days. However, recovery times vary between individuals. - No impact on sexual function:
It does not affect sex drive, performance, or ejaculation. Sterilisation is only confirmed after a follow-up semen analysis shows the absence of sperm.
The NSV technique is considered a reliable option for long-term contraception, but patients should discuss their individual suitability with a healthcare provider.
What is the disadvantage of a no-scalpel vasectomy?
A no-scalpel vasectomy is generally considered a safe and effective procedure, but there are some potential drawbacks to consider:
- Psychological impact:
Some men may worry about the effects on masculinity, even though the procedure does not alter testosterone levels, sexual performance, or libido. - Physical risks:
There’s a small risk of bleeding, infection, or swelling, although studies suggest it may be lower than traditional methods. - Residual sperm:
Sperm can remain in the vas deferens after the procedure, meaning a follow-up semen analysis is required to confirm sterility. Alternative contraception must be used until confirmed clear. - Sperm granuloma:
Leakage from the sealed testicular end can sometimes cause a small, painless lump called a sperm granuloma. This typically subsides on its own, but patients should seek medical advice if concerned. - Long-term discomfort:
Rare cases of mild, long-term discomfort or post-vasectomy pain syndrome may occur, which can often be managed with medical treatment.
Consulting with a doctor can provide clarity about the procedure and its potential long-term effects.
Are there stitches in a no-scalpel vasectomy?
Are there risks involved in a no-scalpel vasectomy procedure?
While a vasectomy without a scalpel is a safe and effective procedure, some risks are associated with it. These risks are usually minor and may occur less frequently compared to traditional methods.
- Mild bleeding or bruising:
Although the procedure uses a small puncture instead of incisions, minor bleeding or bruising around the puncture site can occur in some cases. - Swelling or discomfort:
Some men may experience mild swelling or discomfort a few days after the procedure. This is a common response and typically improves with appropriate aftercare. - Infection:
Although infection at the puncture site is uncommon, it is possible. Keeping the area clean and following aftercare instructions can help reduce this possibility. - Sperm granuloma:
If sperm leaks from the ends tied during the procedure, a small lump may develop. This lump is usually not painless and often subsides over time, but medical advice should be sought if symptoms persist. - Residual sperm present:
After the procedure, sperm may still be present in the vas deferens for a short period. A follow-up semen analysis is required to confirm the absence of sperm. - Occasional long-term discomfort:
A few men may experience mild discomfort after the procedure. This is uncommon and can often be managed with medical guidance.
Despite these risks, the no-scalpel vasectomy is widely considered a reliable option for long-term contraception. Patients should consult a doctor to discuss individual suitability.
Will a no-scalpel vasectomy affect my sexual performance or libido?
Undergoing a no-scalpel vasectomy in Perth does not impact sexual performance or libido. The procedure only affects fertility by blocking the vas deferens to prevent sperm from entering the semen.
Testosterone levels, erections, ejaculation, and sexual desire are not physically altered by the procedure. Some men report feeling more relaxed about sex due to the reduced risk of unintended pregnancy, but individual experiences vary.